UPMC Experience & Organization Design
Bethel Park, Pennsylvania, eight miles south of Pittsburgh, is a middle class suburb with an aging population. UPMC South Hills, a facility built in the 1990s, and had grown to include over a dozen outpatient offices like surgery, cardiology, and primary care. More broadly, UPMC’s network was expanding at the time, opening and acquiring clinics and hospitals across the region.
Our design team was initially asked to examine and improve patient experience at South Hills. After observations, ethnographic research, interviews, and other methods, it was evident that the patient experience was actually one of the facility’s strong suits. Our team worked with management to address another challenge that emerged: a need for stronger overall vision, planning, and unity between South Hills and UPMC Corporate. We delivered a strategic plan and vertical map for how South Hills could become a model for other outpatient facilities.
Roles: Design research, strategic planning, prototyping, service design and organization design.
Collaborators: Alex Cheek, Gabe Clapper, Bridget Lewis; Shelley Evenson, Advisor.
A collaboration between Carnegie Mellon School of Design and the UPMC Center for Quality Improvement and Innovation.
Read Case Study →
Extensive Field Work
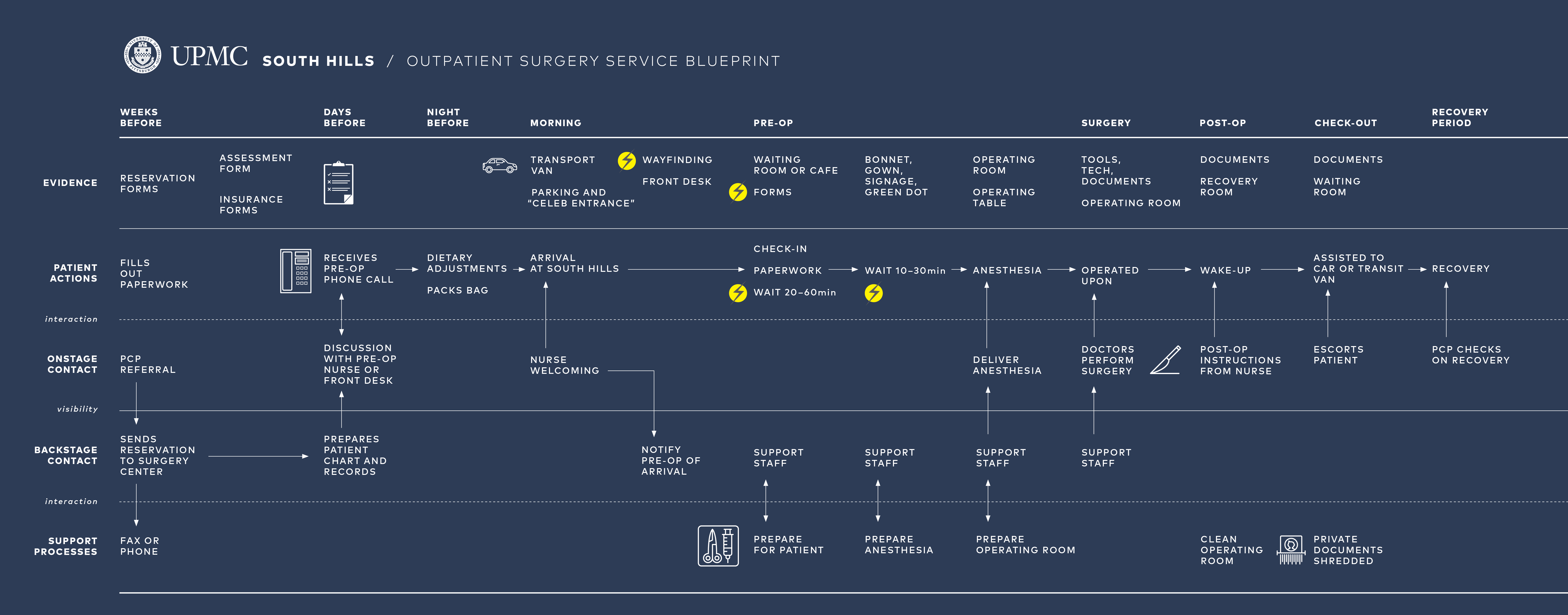


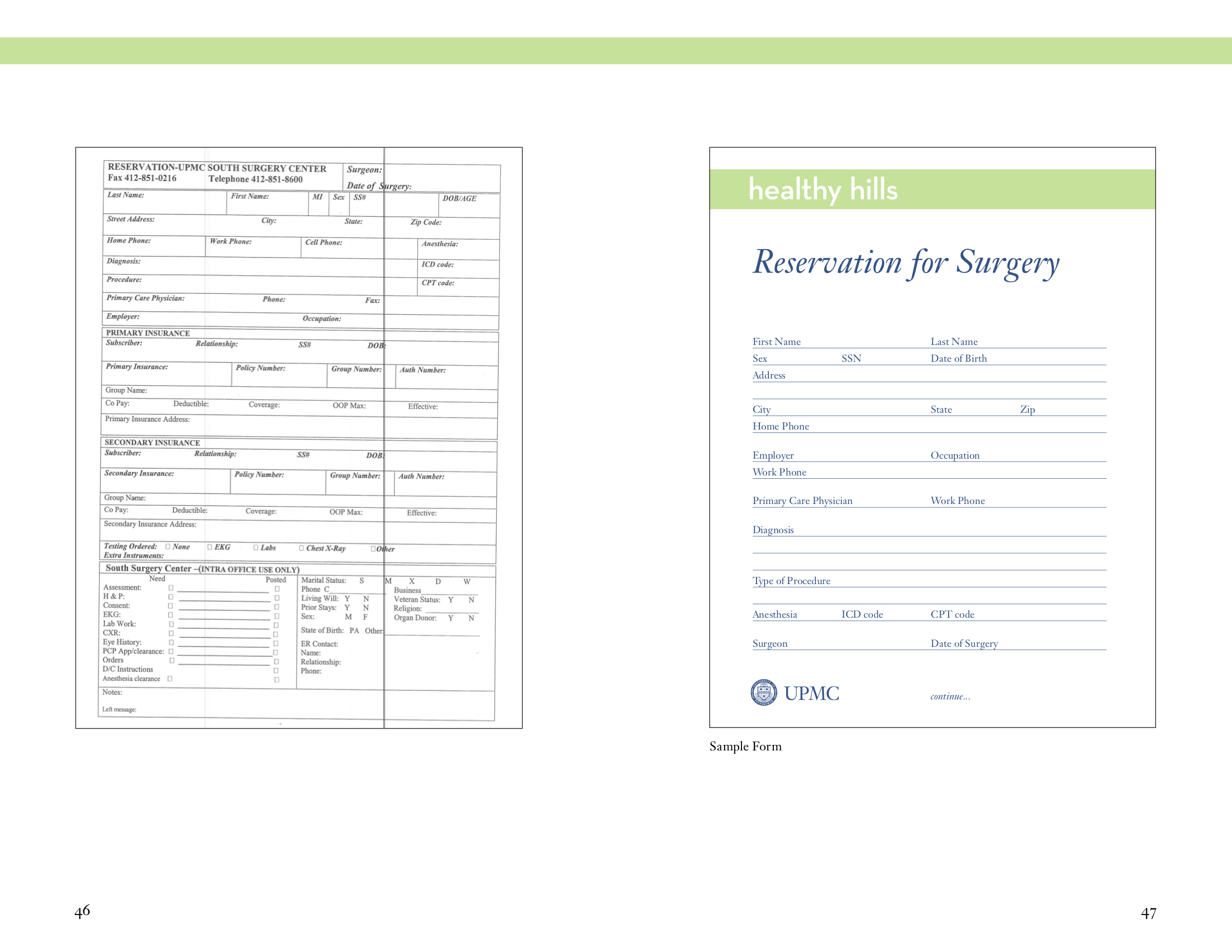
Interviews, shadowing, blueprinting, and surveys were amongst the methods used during the weeks of field work.


We audited wayfinding systems, information flow, records, scheduling, and referrals.

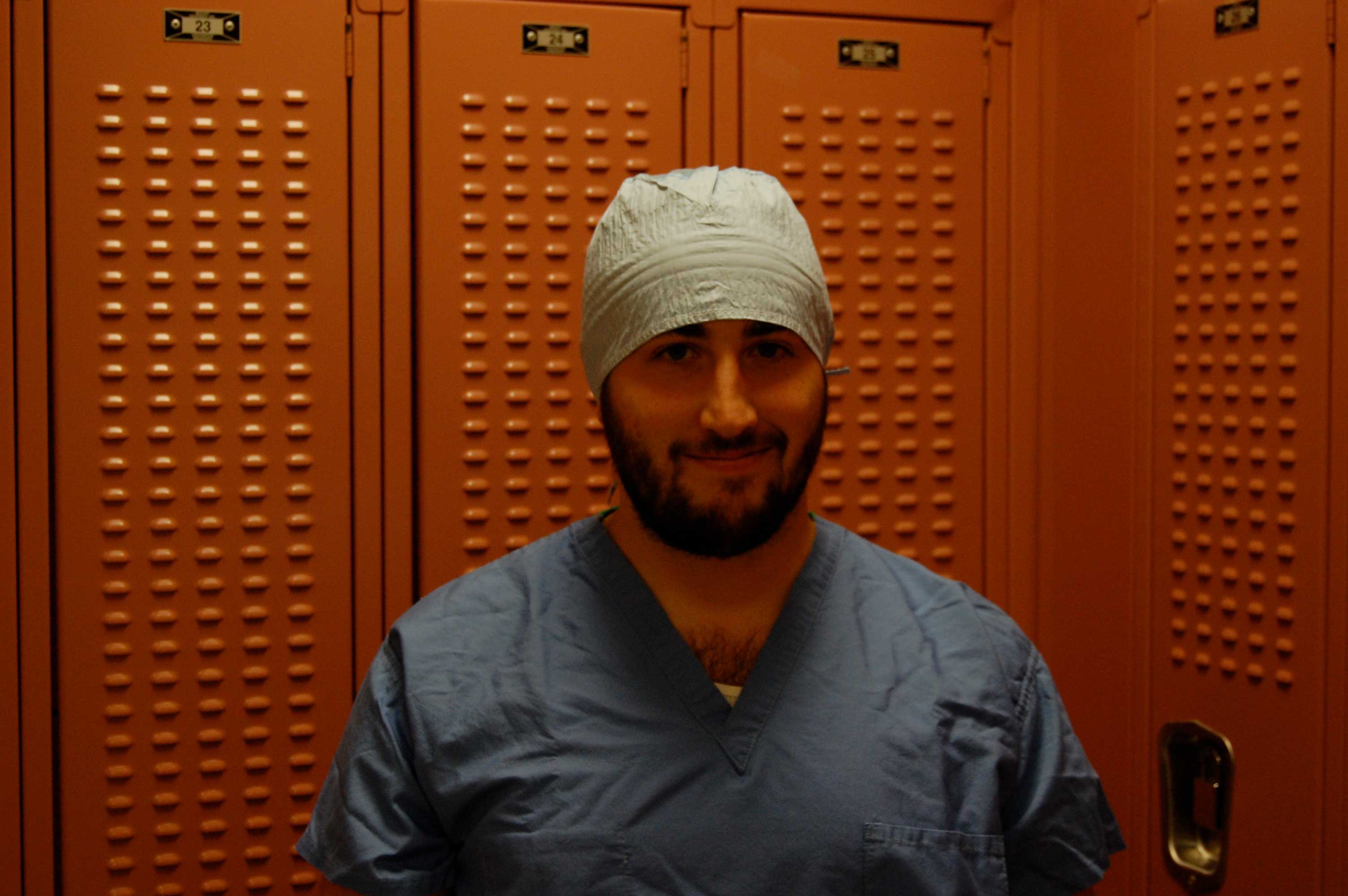
While the directive was to improve patient experience, research indicated high levels of satisfaction across many departments. What was revealed, however, was a lack of cohesion in the facility.

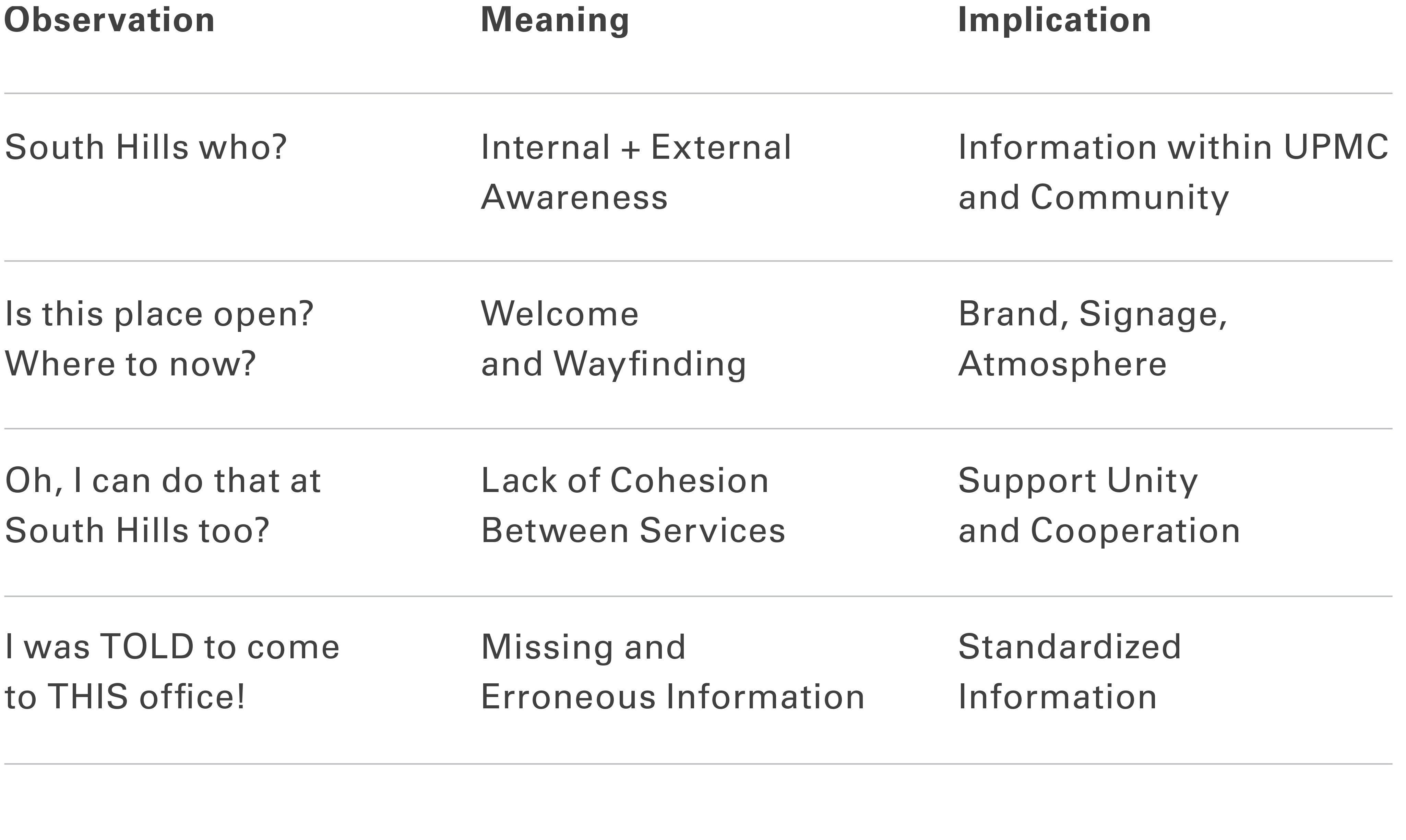
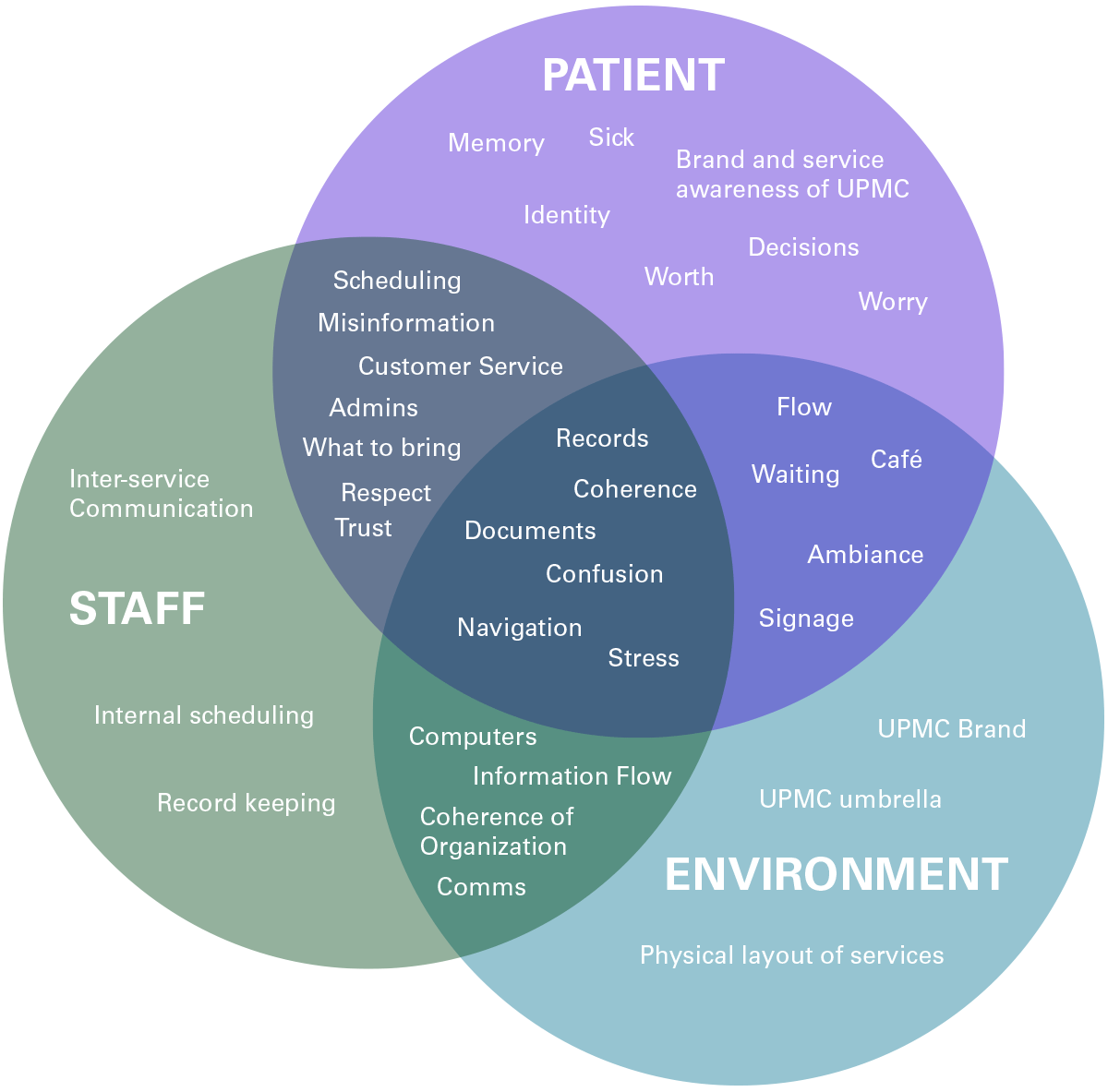
A New Research Method

Understanding “healthcare of the future” begins with understanding people just as much as it does technology and advancements in medicine. For us, it meant leaving South Hills and integrating with the community, starting at a nearby mall on a Tuesday morning. The research was completely informal, unstructured, and randomly selected. We bought coffee for mall-walkers, talked with employees, and recorded their stories. No data came from it aside from the revelation that asking “what does the ‘future of healthcare’ look like to you” yields almost no tangible insights. Like product design, unless people are guided in specific ways to think about the future, they will struggle to articulate it.
We created and employed a remapping technique to understand the values of individuals and community ethos: prompted with a set of four image cards per question, users were asked “if healthcare in the future were” one of the four juicers, one of the four magazines, one of the four vacation spots, one of the four cars, “which one would it be and why?” The choices they made were irrelevant to us; what mattered was their justification: “I like the green juicer because it’s personal. It’s one-at-a-time. With the industrial juicer, I would feel like just another orange.”
Between juicers, vacations, and media, we collected hundreds of data points that spoke to desires of comfort, accessibility, brightness, efficiency, happiness, peace, relaxation, individuality, immediacy, and simplicity. We ran a linguistic analysis and the results helped us construct a vertical map defined by the community itself.

“I like the green juicer because it’s personal. It’s one-at-a-time. With the industrial juicer, I would feel like just another orange.”
Understanding ‘healthcare of the future’ begins with understanding people just as much as it does technology and advancements in medicine. For us, it meant leaving South Hills and integrating with the community.
A Strategic Plan
Vertical maps connect broad, aspirational direction, with principles and goals that can be roadmapped, and tactical projects that can be measured. They help align complex organizations that seek transformation on many levels. They help build a culture of change where all participants have clarity on their role and the shared mission.
The vertical map stemmed from the lack of vision for South Hills and UPMC’s many other satellite facilities. While we could continue to prototype valuable ground-level changes to influence patient experience, they needed to be part of a broader plan, a strategy, and a vision — one that balanced stakeholder perspectives and constraints, patient-centered values, and community ethos.